- Letter from the Editors
- Editorial
- Bloodstream infections in ICU: Classification – Epidimiology - Treatment.
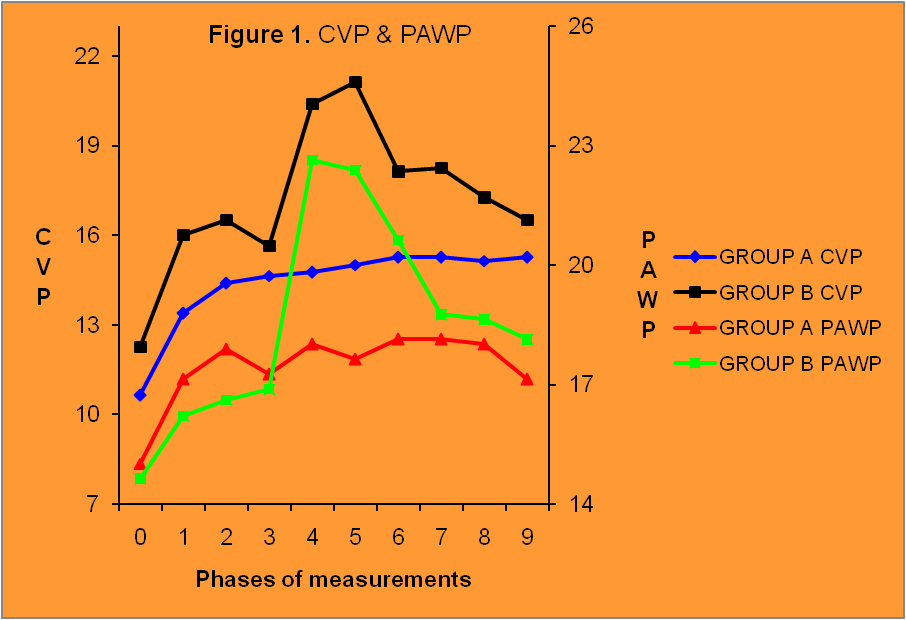
- Cardiovascular effects of increased intra-abdominal pressure in pigs with or without coexistent sepsis.
- Eosinophilia: An early marker of adrenal insufficiencyin critically ill patients with septic shock?
- A rare case of late presentation of infantile hypertrophic pyloric stenosis in a 5-year old child.
- Thymectomy in a patient with thymoma-related myasthenia Gravis and recent recovery from adult respiratory distress syndrome.
Dear colleagues,
In this first issue of the Greek e-journal of Perioperative Medicine for 2018 we are very honored to present -throughout our Editorial- an invitation from the organizing and scientific committee of the ANAESTHESIA 2018 for ANAESTHESIA 2018 – 15th Congress of Anesthesiology and Ιntensive Medicine which is to be held in Thessaloniki, on the 20th to the 23rd of September, 2018.
The present issue, also, covers a wide area of interests. The review article of Schizodimos et al summarizes the classification, epidemiology and management of Bloodstream infections (BSIs). They refer to the therapeutic strategy of Bloodstream infections that should be based on international guidelines in combination with local microbiology and local antibiotic resistance data.
Next, Grosomanidis V et al present an experimental study in order to record the effect of increased intra-abdominal pressure on the cardiovascular system of pigs, with or without additional sepsis. Their results showed that the increase in intra-abdominal pressure was well tolerated by the laboratory animals without septic condition, while in septic animals the increase in intra-abdominal pressure had an unfavorable effect on the cardiovascular system.
The following study of Mouloudi E et al. presents data that showed that relative eosinophilia may be… Continue reading
Certainly, nobody during the autumn of 1990, when the 1st Congress of Anesthesiology & Intensive Medicine was first inaugurated, had any idea of the impact and the influence this new institution would gain in the years to come. This very first congress was under the organizational presidency of Dr. Nikos Balamoutsos, respectable teacher and skillful director in the field.
But this was not a surprise; Thessaloniki had already experienced pioneering in Anesthesiology. Dr. Spyros Makris (1926-1978) was the first ever Professor of Anesthesiology in Greece (1974) at the Aristotle University of Thessaloniki. He wrote the very first textbooks of Anesthesiology in Greek and published more than one hundred papers, in Science, Anaesthesia and Analgesia, and other journals. This is the reason why during the opening ceremony, the honorary lecture has his name and is assigned to an academic with a broader scientific flair, normally from the local medical community.
Continue readingBloodstream infections (BSIs) are a frequent and life threatening condition in hospital settings. The case fatality rate associated with BSI reaches 35-50% when associated with admission to intensive care unit (ICU). The extensive use of intravascular catheters, however, is recognized as the most important factor contributing to the occurrence of BSI. Catheter-related BSIs (CR-BSIs) are the most common types of BSI in ICU. Bacteraemias that occur in the ICU are classified as Community Onset BSI and Hospital Acquired (HA) BSI. They are also distinguished in primary and secondary. Community-onset BSIs are those that occur in outpatients or are first identified 48 h after admission to hospital/ICU, and they may be sub classified further as health care associated (HCA), when they occur in patients with significant prior health care exposure, or community associated, in other cases. Hospital Acquired (HA) and / or ICU-acquired BSIs are defined as those occurring more than 48 hours after the patient's admission into the hospital or ICU or within 48 hours of leaving the hospital or the ICU. Community acquired BSIs usually due to susceptible bacteria should be clearly differentiated from HCA and HA BSIs frequently due to resistant hospital strains. A bedridden status, presence of indwelling devices, recent hospitalization or contact with health care facilities and recent antibiotic therapy may represent the most important risk factors for the development of emerging multi drug resistant (MDR) GN infections. The basic components of the treatment of a bacteraemia in the ICU are determining the type of bacteraemia in order to target potential pathogens, the initiation of empirical antimicrobial therapy based on the guidelines, and the source control if it is a secondary bacteremia. These goals become difficult to achieve in case of BSI due to multi-drug resistant pathogens with high MICs to antimicrobials. The main mechanisms which have put in danger the marvelous antibiotic weapon are the production of ESBL (several different subtypes), the production of carbapenemases and metallo-betalactamases, with consequent spread of multi or pan-resistant organism and the emerging growing resistance in colistin. The targeted treatment should be applied immediately after receiving the susceptibility test from the cultures. Targeted treatment essentially consists in redefining antibiotic treatment, in de-escalation in order to decrease the antibiotic selection pressure, and in determining the duration of treatment. Source control is recognized as an important part of the therapy of BSIs and has been recently shown to be independently related with outcome. Depending on the source of the infection (pneumonia, CRBSIs, urinary tract infections, intra-abdominal infections), the therapeutic strategy should be based on international guidelines in combination with local microbiology and local antibiotic resistance data.
Continue readingIncreased IAP often coexists with sepsis in severely ill patients in the ICU, under mechanical ventilation and pharmaceutical support of the circulation with inotropes and vasoactive drugs. Both conditions have an unfavorable effect on the cardiovascular system. The purpose of this experimental study was to record the effect of increased intra-abdominal pressure on the cardiovascular system of pigs, with or without additional sepsis. Sixteen male pigs were randomly assigned in two groups A and B. In both groups, after induction to anesthesia and mechanical ventilation, the intra-abdominal pressure was increased to 25mmHg by helium insufflation in the peritoneal cavity, and that level of IAP was preserved until the end of the experiment. In Group A no other intervention apart from the increase in IAP was made, whereas in Group B, 60 minutes after the increase in IAP, 100μg/kg LPS were administered. Data were recorded after induction of anesthesia and initiation of mechanical ventilation (baseline measurement/measurement 0) and thereafter every 20 min after intra-abdominal pressure increase. The last measurement (measurement 9) was obtained immediately before release of pneumoperitoneum. Parameters measured or calculated included HR, BP(s,d,m), RVPs, PAP(s,d,m), PΑWP, CO, SV, SVR, PVR, SvO2, ETCO2. HR increased statistically significantly only in Group B, 60 minutes after the administration of LPS. BP (s, d, m) presented a significant change only in Group B, an initial increase immediately after LPS administration, followed by a decrease. CVP, RVPs and PAP (s, d, m) increased in both groups after IAP increase, whereas they presented an additional increase in Group B, after LPS administration. PΑWP changed only in Group B, after LPS administration. CO and SV were dramatically reduced in Group B, immediately after LPS administration, but gradually recovered their initial values until the end of the experiment. SVR changed only in Group B. They increased after LPS administration and then they gradually decreased. PVR increased dramatically after LPS administration and, despite gradual decrease they remained at high values until the end of the experiment. SvO2 decreased in Group B after LPS administration but gradually recovered its initial values. At the conditions of this particular experiment, the increase in intra-abdominal pressure was well tolerated by the laboratory animals. On the contrary, sepsis induction by LPS administration had an unfavorable effect on the cardiovascular system.
Continue readingAdequate adrenocortical function is essential to survive critical illness. The goal of this study was to determine whether eosinophilia could serve as a useful and early marker of adrenal insufficiency in critically ill patients with severe septic shock. During a 1-year period, we prospectively studied 294 ICU patients.16 patients (5.4% of ICU admissions) with eosinophilia more than 3% of the white blood cell count and septic shock unresponsive to adequate fluid and vasopressor therapy, were included. A high dose (250 mcg i.v) corticotropin stimulation test was performed. Eosinophilia (>3%) was diagnosed in 16 patients with vasopressor-unresponsive septic shock. Eosinophilia was present 1.9±0.9d (range 8-96h) before the onset of septic shock. 11/16 patients failed to respond to corticotropin stimulation test above the critical level of 9 mcg/dL rise and 2/16 had baseline cortisol concentration <10 mcg/dL. Baseline cortisol level, maximal cortisol increase post-corticotropin administration and Eosinophils count (%) were higher in survivors (p≤0.05). A hydrocortisone infusion (300mg/d) treatment resulted in haemodynamic improvement in 12 of 16 patients (75%). The 28-day mortality (following the onset of septic shock) was 43.7%. Relative eosinophilia may be considered as a useful and early bioassay for adrenocortical function assessment in critically ill patients with septic shock and assumed adrenocortical depression.
Continue readingThe case describes a late presentation of Infantile Hypertophic Pyloric Stenosis in a 5 year old boy, and its management.
Continue readingThymoma is one of the most common tumors of the anterior mediastinum in adults, arising from thymic epithelial cells. Complete surgical resection is the treatment of choice in myasthenic patients with thymoma. A 41 year-old male, with myasthenia gravis and thymoma was scheduled for thymectomy. Ten months ago, he developed pneumonia. He had a history of pneumonia (10 months ago) complicated by severe adult respiratory distress syndrome (ARDS), managed successfully with a short-term support with extracorporeal membrane lung assist device NovaLung. Long-term impairments in lung volume and diffusion capacity have been reported in adult respiratory distress syndrome survivors. Total intravenous anesthesia technique and especially muscle relaxants infusion require special attention in this group of patients. Our management strategies in this case included careful assessment of respiratory function, avoidance of premedication, use of short-acting anesthetic agents (propofol, remifentanil), use of suggamadex for reversal of rocuronium-induced neuromuscular block, and intraoperative monitoring with a train-of-four monitor and monitoring in an intensive care unit for 24 hours after surgery.
Continue reading