Authors: Asteriou Ch, MD, MSc, PhD, Lazopoulos A, MD, Rallis Th, MD, Gogakos AS, MD, Paliouras D, MD, MSc, PhD, Barbetakis N, MD, PhD
ABSTRACT
Schwannomas, known also as neurilemmomas, are considered to be benign in the vast majority of cases. Originating from the schwan cells of the neural sheath of peripheral nerves, they usually develop in the head and neck. Involvement of the brachial plexus is relatively rare, with an incidence of 0.3–0.4/100,000 person per year1. Malignant transformation is extremely uncommon. Patients’ initial symptoms include pain, loss of function, numbness or a progressively growing mass in the supraclavicular region. Neglected cases regarding larger benign tumors may present with monoparesis of an upper limb2. Primary malignant schwannomas of the brachial plexus causing monoplegia are extremely infrequent and to the best of our knowledge very few cases have been published in the international literature.
CASE PRESENTATION
A 46 year old female patient was admitted to our hospital complaining for a painful, progressively enlarging palpable mass in the left supraclavicular region since 14 months. Over the last 7 months she was suffering fromnumbness of the left upper limb together with progressive weakness in the left hand. Gradually, almost complete loss of function of the left upper limb was established with subsequent inability to perform any task. The movements of the left upper limb were limited to a great extent. The rest of her medical record was clear. Neurological examination revealed serious motor and sensory deficits. Marked hypotonia was recorded in the left upper limb. Extreme wasting and weakness of muscles was noted. Sensory modalities for touch, temperature and pin prick were lost.
The routine imaging studies did not reveal anything abnormal. Magnetic Resonance Imaging (MRI) was consistent with a mass encasing the left brachial plexus (Figure 1A and Figure 1B). The appearance of the depicted mass, measuring 3.34 X 2.36 cm raised the suspicion of a nerve sheath tumor. Computed Tomography (CT) scans of the thorax, abdomen and brain as well as the bone scan were negative for metastases. CT guided Fine Needle Aspiration Cytology (FNA Cytology) was inconclusive.
A partial sternotomy from the jugular notch to the level of the left third intercostal space with a vertical extension along the third intercostal space was performed. After careful dissection the tumor was recognized to infiltrate the left brachial plexus (Figure 2A). Both intraoperative nerve stimulator and electromyography (EMG) revealed complete loss of function of median, ulnar, radial and musculocutaneous nerves. Radical excision of the tumor en bloc with the affected segment of the left brachial plexus was executed (Figure 2B). Pathological examination in combination with immunohistochemical analysis revealed a malignant schwannoma infiltrating the brachial plexus (Figure 2C). Dissection margins were free of malignancy. The postoperative period was uneventful and the patient was discharged on the seventh postoperative day.
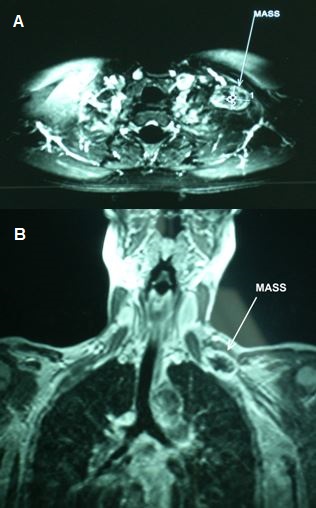
Figure 1: A: Axial Magnetic Resonance Image depicting a mass involving the left brachial plexus and measuring 3.34 cm in the long axis (white number 1) and 2.36 cm in the short axis (white number 2). B: Coronal Magnetic Resonance Image showing the same mass in relation with the adjacent anatomic structures.

Figure 2: A: Intraoperative view of the tumor infiltrating the left brachial plexus. B: Surgical specimen C: Pathological examination of the specimen (malignant schwannoma). High power showed in better detail the malignant appearance of the nuclear pattern within the spindle cells of this malignant schwannoma that is strongly positive with the S100 immunohistochemical analysis
DISCUSSION
Schwannoma of the brachial plexus is a rare entity. It usually appears as a benign well encapsulated mass originating from the nerve sheath. Involving symptoms attributed to nerve compression should raise suspicions and further evaluation with MRI should follow. Surgical enucleation of this benign tumor is the treatment of choice in order to relief patient’s symptoms and prevents or minimizes a possible neural damage due to tumor’s enlargement and compression of the valuable adjacent structures. Complete resection while preserving the vital surrounding nerves is feasible in the majority of cases3.
However, in the extremely rare case of a malignant schwannoma of the brachial plexus the mainstay of treatment is radical surgical excision. The primary goal of the operation is to achieve complete surgical resection of the tumor with negative margins. This offers the best outcome with respect to both local recurrence and distant metastases4.
Radiation therapy has become an integral part of local disease control in most cases. In combination with wide surgical excision, radiation therapy offers possible survival advantage5. Chemotherapy is intended for systemic disease which is either too small to detect or too diffuse, rendering local treatment techniques ineffective. The use of chemotherapy is only employed in high-grade disease, in which metastatic disease is likely. Large, deep, high grade tumors and tumors which demonstrate metastases or metastatic potential are typical indications for chemotherapy treatment 4,5.
Recurrence can be discussed in terms of local disease and distant or metastatic disease. The local recurrence rate for Malignant Peripheral Nerve Sheath Tumors (MPNSTs) has been reported to range from 40-65% and the distant recurrence rate has similarly been reported to range from 40-68% 4. Five-year survival has been reported to range from 16-52% 4. Longer survival has been correlated with complete surgical excision, small tumor size (<5cm), and the presence of a low grade component5.
REFERENCES
- Ganju A, Roosen N, Kline DG, Tiel RL. Outcomes in a consecutive series of 111 surgically treated plexal tumors: a review of the experience at the Louisiana State University Health Sciences Center. J Neurosurg 2001; 95(1):51-60.
- Patel ML, Sachan R, Seth G, Radheshyam. Schwannoma of the brachial plexus:a rare cause of monoparesis. BMJ Case Rep, doi: 10.1136/bcr-2012-008525.
- Rashid M, Salahuddin O, Yousaf S, Qazi UA, Yousaf K. Schwannoma of the brachial plexus; report of two cases involving the C7 root. J Brachial Plex Peripher Nerve Inj2013; 8(1):12.
- Kourea HP, Bilsky MH, Leung DH, Lewis JJ, Woodruff JM. Subdiaphragmatic and intrathoracic paraspinal malignant peripheral nerve sheath tumors: a clinicopathologic study of 25 patients and 26 tumors. Cancer1998; 82(11):2191-2203.
- Wong WW, Hirose T, Scheithauer BW, Schild SE, Gunderson LL. Malignant peripheral nerve sheath tumor: analysis of treatment outcome. Int J Radiat Oncol Biol Phys1998; 42(2):351-360.
Author Disclosures:
Authors Asteriou Ch., Lazopoulos A., Rallis Th., Gogakos A.S., Paliouras D., Barbetakis N. have no conflicts of interest or financial ties to disclose.
Corresponding author:
Christos Asteriou,
Al. Symeonidi 2, 54007,
Thessaloniki, Greece,
tel: +302310898314,
e-mail:









