- Letter from the Editors
- Editorial
- Ενδοκράνια Υπέρταση. Παθοφυσιολογία – Κλινική εικόνα – Παρακολούθηση.
- The clinical applications of body weight and endotracheal tube size prediction formulas in pediatric patients.
- Χρήση υπηρεσιών του Εθνικού Κέντρου Άμεσης Βοήθειας από δομές φιλοξενίας προσφύγων -στοιχεία 6 μηνών- από τη Βόρεια Ελλάδα.
- Anesthetic management of a patient with Myasthenia Gravis for abdominal surgery
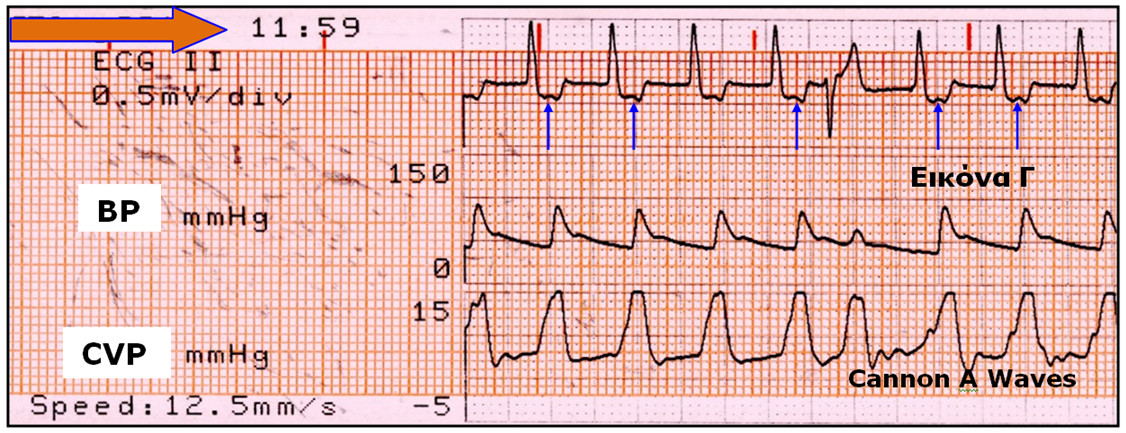
- Σύνδρομο Βηματοδότη σε Προσωρινή Επικαρδιακή Βηματοδότηση μετά από Αορτοστεφανιαία Παράκαμψη: Παρουσίαση περιστατικού και ανασκόπηση της βιβλιογραφίας.
Dear colleagues,
The uninterrupted and continuous presence of the Greek e-journal of Perioperative Medicine in the scientific literature, over last 17 years, has been gradually increased and this is attributed to your help. On behalf of the editorial board, we would like to emphasize that our goal is ensure free-access, high quality, published articles in the area of medical press and we would like to thank you again for this continuous support. This is the third (3rd) issue of the year and our goal is to raise the issues from three to four per year. The participation of all of us with high quality publications will enable our journal to continue to be part of international libraries.
The present issue covers a wide area of interests. The review article of Schizodimos et al summarizes the major pathogenetic mechanisms, the clinical manifestations and the monitoring techniques of intracranial hypertension. They refer to 2016 Guidelines for the Management of Severe Traumatic Brain Injury, where a measured ICP above 22 mmHg is considered an indication for intervention. They also describe the major pathogenetic mechanisms of intracranial hypertension (venous occlusion, increased cerebral volume, increased… Continue reading
The exchange of experiences and ideas among colleagues remains the key of scientific progress. In fact, knowledge is a sum of gathered experiences and education is nothing more than an attempt to pass all those knowledge to the next generation.
In rapid transforming scientific disciplines like medicine, the need for this exchange is essential. The latter can take different forms. Oral conversation may seem like the humble way of communication. Nevertheless, “conversation is a meeting of minds with different memories and habits. When minds meet, they don’t just exchange facts; they transform them, draw different implications from them, engage in new trains of thought. Conversation doesn’t just reshuffle the cards; it creates new cards”1-2.
Written documentation, in form of abstracts/posters/articles, is the formal way of medical communication. The ultimate goal: better clinical medicine and thus, better outcomes. Secondary goals: scientific research boost, professional progress, academic career evolution, financial remuneration, etc.
Continue readingIncreased intracranial pressure (ICP) is a serious final common pathway of a variety of neurologic injuries. Elevated ICP has consistently been associated with a poor outcome. It is a medical emergency requiring immediate intervention to prevent permanent damage to the brain. The Monro-Kellie doctrine states that the intracranial space is a fixed volume inside the skull. It describes the principle of homeostatic intracerebral volume regulation. The Monro-Kellie hypothesis and cerebral dynamics are important in order to understand the pathophysiology of intracranial hypertension. Venous occlusion, increased cerebral volume, increased blood volume, mass effect and cerebral edema are the major pathogenetic mechanisms of intracranial hypertension. The clinical manifestations of increased ICP are varied and unreliable. Headache, vomiting, disorientation, and lethargy are the main symptoms as well as symptoms and signs caused by cerebral herniation. ICP monitoring is widely used in clinical practice in order to improve patient outcome. It is especially useful as a robust predictor of cerebral perfusion, and can help to guide therapy and assess long‑term prognosis. Intraventricular catheters remain the gold standard for ICP monitoring, as they are the most reliable, accurate and cost‑effective, and allow therapeutic cerebrospinal fluid drainage. Intraparenchymal catheters are usually considered accurate, with the potential disadvantage that they measure localised pressure, which may not be reflective of global ICP. Furthermore, non‑invasive methods of ICP monitoring, such as transcranial Doppler, optic nerve sheath diameter, etc., have emerged as promising techniques for screening patients with raised ICP in settings where invasive techniques are either not feasible (patients with severe coagulopathy) or not available (setups without access to a neurosurgeon).
Continue readingThere are various formulas and algorithms for the prediction of body weight and appropriate ETT size, in pediatric patients. Body Weight estimation is of paramount importance in pediatrics, especially in emergencies. Predicting the appropriate size of the endotracheal tube saves time, money and reduces complications. The goal of this study was to evaluate the validity of two commonly used formulas for predicting the body weight and the size of the appropriate endotracheal tube, both based on age.353 consecutive pediatric surgical patients aged 2 to 12 years, who required general anesthesia and oral endotracheal intubation were included in this study. Patients were stratified according to their age in two groups: group 2-5 (79 children, 2 to 5 years) and group 6-12 (274 children, 6 to 12 years). At the end of surgery an anesthesiologist, who was not involved in the perioperative treatment, recorded the demographic data and also the size and type of the endotracheal tube used. The prediction of Body Weight (BW) was made according to the following formula: 2-5 y.o.: Weight (kg) = (2 x age in years) + 8 and 6-12 y.o.: Weight (kg) = (3 x age in years) + 7. The formula for calculating the size (size= internal diameter=I.D.) of the endotracheal tube (ETT) was: I.D. for cuffed ETT (mm) = (age / 4) + 3.5 and I.D. for uncuffed ETT (mm) = (age / 4) + 4. For all statistical tests p value <0.05 was considered as statistically significant. In all patients as sum and in both age groups, the predicted body weight was significantly (p<0.05) lower than the actual (measured) weight. In group 2-5y.o, 74.7% of patients received cuffed ETT In group 6-12y.o. 100% of patients received cuffed ETT. In group 2-5 y.o, all patients showed a significantly (p<0.05) lower predicted internal diameter of the ETT, either cuffed or uncuffed, compared to ETT ultimately used. In group 6 -12y.o, there was no statistically significant difference between the predicted and the actually used ETT size. The prediction of body weight in children, by the use of the particular formula, led to underestimation. In children aged 2 to 5 years, the application of the inner diameter calculation of the ETT formula also underestimated the appropriate ETT size. It seems that the traditional age-based formulas often fail to predict the correct ETT size in smaller children which probably does not seem to apply to older children.
Continue readingThe health system’s response characteristics to any refugee crises have special characteristics. Optimal and flexible use of health services is essential in order to meet the needs that arise. Greece has been at the center of such crisis in the last 3 years. The purpose of this study is to record the emergency refugees' transports carried out by the National Center of Emergency Care (“ EKAB”) of Thessaloniki during a 6 months period. In a retrospective study, selected data for the use of emergency care service by the refugees’ camps around Thessaloniki were recorded and analyzed. Parameters included the date, time and location of the incident, patient demographics, callers’ status and incident type. Data on refugee flow in Greece was also included for the same period. Data from 1916 records were analyzed, the majority of which were ages up to 45 years (> 70%). Time distribution of the data displayed increased transport during the first 3 months of the study, followed by a steady decrease. Most of the transports were carried out during the last 3 days of the week. In comparison with the general population, high incident of pediatric cases were recorded. Trauma cases were also high, (35%) - with equally high rates of crime-related injuries. Finally, many ambulance transports were carried out due to delivery or early pregnancy-related problems. Young people and children are the most frequently users of ambulances’ transport from refugee hosting camps. However, due to the complexity of the problem and the dynamic nature of the camps’ population composition, more studies are needed in order to properly evaluate the use of each sector of the health system by refugees.
Continue readingThis case report focuses on the anesthetic management of a patient with Myasthenia Gravis who underwent left-sided colectomy, due to the presence of a tumor on the left colic (splenic) flexure. Myasthenia gravis is a chronic autoimmune neuromuscular disease which is characterized by differ-ent degrees of weakness of skeletal muscles. The anesthetic management and treatment of every patient with myasthenia gravis should be performed carefully, due to the fact that many periopera-tive complications may occur. In our case anesthetic technique included the combination of general anesthesia, with the use of neuromuscular agent and thoracic epidural blockade with the use of a catheter, which permitted intermittent boluses doses and continuous infusion of local anesthetics and opioids. Neuromuscular blockade was reversed with the use of sugammadex. Patient’s periop-erative management was effective and uneventful.
Continue readingThe deficiency of the natural heart pacemaker, the conduction disturbances and the appearance of arrhythmias are common complications after cardiac surgery. Placement of epicardiac electrodes (ventricular, atrial, or both) during cardiac surgery remains common practice, even though few patients will actually need some kind of temporary epicardiac pacing for various periods of time. Temporary epicardiac pacing may be ventricular, atrial or atrioventricular, depending on the specific features of each patient and it aims at preserving the cardiac rhythm, securing the desired heart rate and achieving an acceptable cardiac output. Temporary epicardiac pacing is not without danger, since, under specific circumstances, it may have a negative impact on the hemodynamics of the patient, to the point of circulatory collapse. It may also cause ventricular tachycardia (R on T phenomenon) and cardiac arrhythmias (if pacing is not synchronized to the heart’s natural pacemaker). Ventricular Pacing and Sensing (VVI) is accomplished by the placement of electrodes only on the ventricles, which a priori means a certain degree of hemodynamic compromise, due to the loss of atrial contribution in preserving cardiac output. In certain occasions, this impact may be even more significant. This case report concerns a patient who underwent Coronary Artery Bypass Grafting (CABG) and after placement of the electrodes of temporary epicardiac ventricular pacing he presented significant decrease in systemic arterial pressure and the appearance of cannon A waves on central venous pressure (CVP) tracing every time the pacemaker was triggered. These phenomena, which receded after the disconnection of the pacemaker, consists a case of Pacemaker Syndrome.This problem was solved by adjusting the pacemaker’s frequency at a rate lower than that of the patient’s natural pacemaker.
Continue reading