One half of cortical thymoma patients develop myasthenia gravis (MG), an autoimmune disease affecting the voluntary muscles, while 15% of MG patients have thymomas. Thymectomy has been a mainstay in the treatment of myasthenia gravis and the management of such surgical patients is extremely demanding both at the physician’s and at the nurse’s level. In this paper we review some of the nursing interventions for patients with MG undergoing surgical removal of the thymus gland.
Continue reading

During recent years the application of non invasive ventilation (NIV) has emerged as a central component of respiratory failure management, acute and chronic. Although the use of NIV in acute respiratory failure was initially meant to be given in critical care units, it is nowadays natural to provide it in other settings as well, provided that there are the necessary resources and expertise. NIV represents a viable alternative to endotracheal ventilation and despite most data refer to patients with chronic obstructive pulmonary disease; its indications are continuously expanding to cover more clinical scenarios. Randomized controlled studies are needed in order to provide sound evidence regarding optimal patient-ventilator interface, NIV duration and ventilation parameters in thoracic surgery patients.
Continue readingThe objective of postoperative pain management after thoracotomy is the prevention of postoperative complications, the reduction of the length of hospital stay, the increase of the patient’s satisfaction and finally the resumption of the daily living’s normal activities.
Thoracic surgery affects postoperative respiratory function, along with a high risk of developing postoperative pulmonary complications. Pain is a subjective experience. Postoperative pain management in thoracic surgery patients should be individually applied, based on a well-organized health care system that emphasizes consistent nursing education regarding proper pain management techniques, with an effective communication between the patient and members of the existing multidisciplinary team, especially the nursing staff.
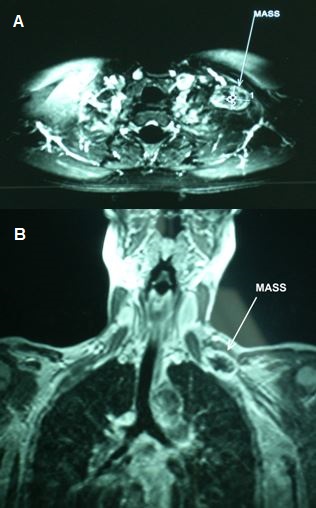
Continue readingSchwannomas, known also as neurilemmomas, are considered to be benign in the vast majority of cases. Originating from the schwan cells of the neural sheath of peripheral nerves, they usually develop in the head and neck. Involvement of the brachial plexus is relatively rare, with an incidence of 0.3–0.4/100,000 person per year1. Malignant transformation is extremely uncommon. Patients’ initial symptoms include pain, loss of function, numbness or a progressively growing mass in the supraclavicular region. Neglected cases regarding larger benign tumors may present with monoparesis of an upper limb2. Primary malignant schwannomas of the brachial plexus causing monoplegia are extremely infrequent and to the best of our knowledge very few cases have been published in the international literature.
Continue readingSyncope is a common complaint in clinical medical care. Except of neurological disorder, most of the patients havea brief benign clinical course with spontaneous recovery. Etiology may range from benign disorders to severe life-threatening diseases.Syncope as the leading symptom in patients suffering from intrathoracic neoplasm is uncommon. A rare case of a giant pleural solitary fibrous tumor causing recurrent episodes of syncope is presented. Diagnostic considerations and therapeutic strategy are discussed.
Continue readingSeveral techniques have been described for percutaneous internal jugular vein catheterization. Some of them are associated with complications, such as tracheal tube cuff puncture. We describe two cases of this rare but potential devastating complication, after which our patients recovered uneventfully
Continue reading