- EDITORIAL
- MECHANICAL VENTILATION IN ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS)
- HISTORY AND EVOLUTION IN CARDIAC ANESTHESIA
- INTRAOPERATIVE PULMONARY HYPERTENSION: ETIOLOGY ANDMANAGEMENT BASED ON MONITORING OF PULMONARY CIRCULATION
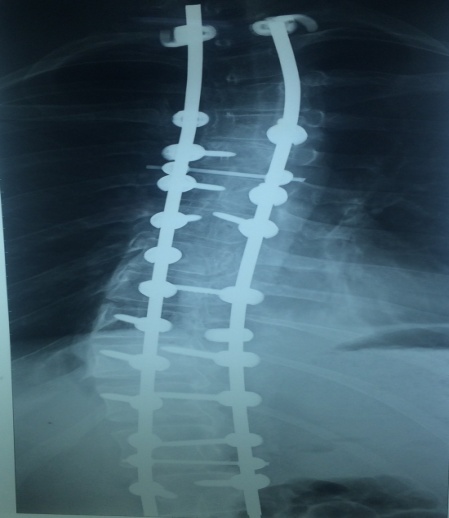
- PULMONARY EMBOLISM FOLLOWING ADOLESCENT IDIOPATHIC SCOLIOSIS CORRECTION SURGERY: A CASE REPORT
- CONVERSION DISORDER: TETRAPLEGIA AFTER SPINAL ANESTHESIA
The first issue of 2017 contains few, but very interesting articles. In their review Shizodimos et all, highlight the details hidden in the available literature about mechanical ventilation in Acute Respiratory Distress Syndrome, which after publication of Berlin definition1, is gaining again more and more interest2.
In the next article, Karveli –Argyriadou challenge the current trend regarding cardiac anesthesia publications by presenting us its track in time. In the era of minimal invasive cardiosurgery, genetic therapy and ultra-fast track cardiac anesthesia protocols, they remind us the course and the moments of its evolution and allow us to “look back in order to realize how much we have progressed”.
Papapostolou et al, focus on the importance of right interpretation of hemodynamic monitoring and present 3 cases of acute intraoperative pulmonary hypertention during cardiac surgery.
The last two articles describe a case on pulmonary embolism after surgery for Adolescent idiopathic scoliosis and a conversion disorder that was presented with tetraplegia post spinal anesthesia.
Continue readingAcute respiratory distress syndrome (ARDS) is an acute inflammatory lung injury, associated with increased pulmonary vascular permeability, increased lung weight, and loss of aerated lung tissue. There remains limited information about the epidemiology, recognition, management, and outcomes of patients with the ARDS, but in-hospital mortality is still high for those with moderate and severe ARDS (40.3% and 46.1%, respectively). Mechanical ventilation does not cure ARDS but simply buys time by maintaining a gas exchange sufficient for survival. The guiding principle of mechanical ventilation of ARDS is the new setting is less harmful to the lung structure than the previous one, thus avoiding the ventilator induced lung injury (VILI). Among outcome studies testing different tidal volumes, only the study comparing the two extreme values tested (6 mL/kg versus 12 mL/kg) showed a significant benefit of lower tidal volume. ‘The best positive end expiratory pressure (PEEP)’ does not exist. Recruitment maneuvers (RMs) are helpful in increasing aerated lung volume, which decreases strain and tidal recruitment/derecruitment. There is no definitive evidence regarding the clinical effectiveness of RMs to improve clinical outcomes of ARDS patients, although RMs may decrease the mortality of patients with ARDS without increasing the risk for major adverse events. There is no evidence for a difference between pressure control versus volume control ventilation in terms of physiological outcome or mortality. The effect of respiratory rate on the occurrence of VILI or outcome in ARDS has not been independently studied. Increasing inspiratory time has been suggested to improve oxygenation. Prone position (PP) is a standard practice in clinical treatment of ARDS patients to improve systemic oxygenation to any patient with moderate or severe ARDS as it may confer a statistically significant mortality advantage. There is evidence that neuromusculal blockade by cisatracurium besylate has an outcome benefit in ARDS patients since they improve lung mechanics and lung inflammation. Optimal dosing and monitoring strategies will need to be further studied.
Continue readingCardiac surgery is a specialty with a relatively short history. The difficulties and particularities of Cardiac Surgery made apparent right from the beginning that there was a need forspecialized anesthesiological support. In 1940, Cardiac Surgeons pioneers recognized the role and contribution of cardiac anesthesiologists. In 1945, Blalock thanking his anesthesiologist co-workers Lamont and Harmel in public and mentioned that thanks to their anesthesiological support there “was no death during the first 55 operations”. Russell Brock, in 1949, highlighted the importance of collaboration between cardiac surgeons and cardiac anesthesiologists and mentioned “In this type of surgeries co-operation is necessary. The anesthesiologist plays a vital role and deserves special honor and recognition.” Since the first application of the electrocardiogram to operating theatres in 1950, the introduction of transesophageal echocardiography perioperatively in 1971, until the last decade with the application of coagulation monitoring, the newer data in the management of severe bleeding and the anesthesiological support in brand new minimal invasive techniques, cardiac anesthesiologists have vitally supported the evolution of cardiac surgery. The following text is a historical review describing the contribution of cardiac anesthesia in a continuing effort to improving clinical outcome and enhancing the safety of cardiac surgery.
Continue readingEvaluation of monitoring readings, taking into account each patient’s pathology as well as the impact of every medical intervention can guide us to make optimal clinical decisions in the periopeative setting. We present three cases in which clinical decisions concerning the management of acute perioperative pulmonary hypertension were based both on haemodynamic monitoring readings and on each patient’s specific pathology. First case: After anesthesia induction in a patient with severe aortic valve insufficiency, an increase in pulmonary artery pressure was recorded. Infusion of isoprenaline, which has a positive chronotropic effect, decreased diastolic time, diastolic blood flow into the left ventricle and also pulmonary artery pressure. Second case: A patient with severe aortic valve stenosis was found with increased pulmonary artery pressure. Intravenous administration of atenolol (1+1mg) reduced the heart rate and the pulmonary artery pressure. Third case: A 15 year old patient with aortic isthmus rupture underwent open surgical repair with graft interposition. After establishment of one lung ventilation and left thoracotomy, pulmonary artery pressure increased. Pulmonary hypertension was managed successfully by oxygen insufflation to the non-ventilated left lung. In our first patient, heart rate increase reduced diastolic time, which decreased the amount of retrograde blood flow into the left ventricle through the regurgitant aortic valve. In the second patient, the heart rate reduction decreased blood flow velocity through the stenotic aortic valve as well as the pressure gradient between left ventricular chamber and aorta. In both patients, enhanced left ventricular function resulted in a reduction in pulmonary artery pressure. Decrease of the alveolar partial pressure of oxygen (PAO2) is the most important parameter that stimulates hypoxic pulmonary vasoconstriction. Oxygen insufflation increased PAO2, resulting in a decrease in pulmonary artery pressure .Clinical decisions based on haemodynamic monitoring readings resulted in effective management of pulmonary hypertension and in a good patient outcome.
Continue readingScoliosis is a musculoskeletal disorder, in which there is a sideways curvature of the spine. Surgical correction of scoliosis is a long-lasting high-risk procedure, which can lead to serious complications such as pulmonary embolism and substantial haemorrhage. In our case a 20 year-old male with idiopathic scoliosis curve of 82o underwent a reconstructive spinal surgery. Tranexamic acid (TXA) i.v infusionwas used intraoperatively to reduce the blood loss. The operation took 8h to complete and proceeded well without complications. Afterwards the patient was then transferred to ICU. The third postoperative day he was admitted back to the orthopedic ward. 7h after admission he presented clinical symptoms of pulmonary embolism (PE). The suspicion of a pulmonary embolism was confirmed by an emergency CT pulmonary angiogram. Consequently, the patient was again admitted to the ICU and was treated with LMWH in a therapeutic dose. Three days later he returned back to the orthopedic ward clinically stabilized and with normal ABGs. In this case report the cause and origin of pulmonary embolism was not clear. The patient was treated with chemical thromboprophylaxis (LMWH) from the first postoperative day and yet PE was not prevented.This event contradicts the supposed rarity of PE after correction of AIS surgery. It also results in a controversy over the efficacy of LMWH on reducing the incidence of VTE and over the safety and proper dosing of TXA.
Continue readingThis case report describes the rare occurrence of tetraplegia, caused by conversion disorder, in a patient who received spinal anesthesia for arthroscopic surgery. A 35-year-old female with a history of migraine headaches received spinal anesthesia for arthroscopic left knee surgery. On sensory block examination, she was noted to have a T10 level of blockade. During surgery and45 min after performing spinal anesthesia, patient reported bilateral loss of both sensation and motor function of her upper limbs. Patient was hemodynamic stable with absence of respiratory depression or any alteration of consciousness level. Physical signs and symptoms did not correlate with any known anatomical or neurological patterns. MRI imaging revealed no abnormalities. Psychiatric consultation was performed wherein familial stressor circumstances were identified, leading to diagnosis of conversion disorder.
Continue reading