The aim of this study was to evaluate resuscitation skills and knowledge of the nursing staff of University Hospital “AHEPA”, who have previously successfully participated in a validated training CPR/AED course, held in ourhospital.In our study 60 professionally active nurses were involved. After completion of a predesigned questionnaire, they were expected to respond to a simulated cardiac arrest-CA scenario in an area where automated external defibrillation-AED was available. The questionnaire consisted of several questions regarding demographic data, participant’s personal opinion on the resuscitation training program, CPR performance and nurse’s attitudes when facing a CA. Participants were evaluated according to the European Resuscitation Council assessment form for basic life support-BLS with the use of AED (consisting of performance in 17 skills).The vast majority of the study population were female nurses (86.7% and 83.3% respectively), 41-50 years old (70%) with more than 21years working experience (53.3%).
Continue readingThe Fontan procedure and its modifications is the definitive therapy for a number of congenital heart diseases. Anesthesia for semi-elective Caeserian section in a pregnant woman with a history of such surgery history can be a real challenge due to probability of high perioperative morbidity and mortality. We present the anesthetic management of a young parturient with a history of a partially repaired complex cyanotic congenital heart disease and perform a literature review.
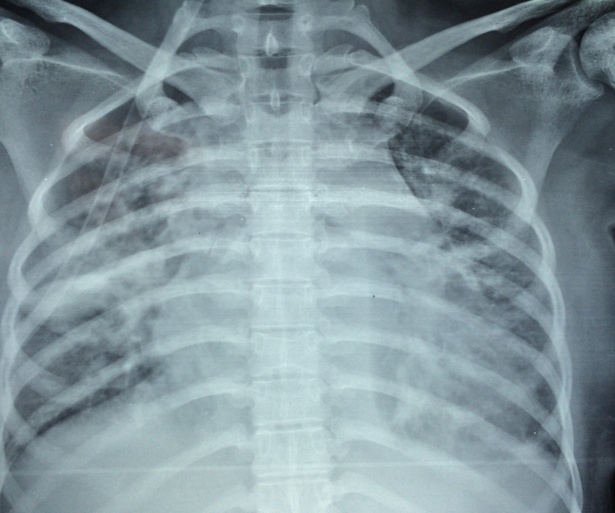
Continue readingAcute Chest Syndrome (ACS) is a rare but often fatal complication in patients with micro-drepanocytic anemia as in those with beta Sickle Cell Disease (SCD). This case report refers to a female patient with known micro-drepanocytic anemia who was admitted to our ICU due to ACS. Treatment included RBC transfusions with WBC reduction, administration of FFP and plasmapheresis within 48 hours from the ICU admission. At the 3rd ICU day, HbA2 level was found elevated up to 77%. The following ICU days, the patient presented absence of the white series of the blood’s cellular components. After twelve days in the ICU the patient died due to hemodynamic shock and herniation of the brain stem. Given that sickle cell crises are potential precursors of this deadly syndrome, everyday practice should prioritize the prevention of sickle cell crises developing into ACS.
Continue readingNeurologic complications after liver transplantation are quite common, with central pontine myelinolysis (CPM) being a rare but fatal complication. In this report, we describe the case of female liver transplant recipient who developed CPM after orthotopic liver transplantation (OLT).A 62-year old woman was admitted to the ICU for postoperative recovery after OLT. The procedure was described as uneventful. The patient had a history of decompensated cirrhosis, tension ascites, class I hepatic encephalopathy and chronic hyponatremia which necessitated repeated hospitalizations in the year prior to transplantation.The patient was unable to be weaned from ventilator support and did not show an improvement in mental status (GCS=5) despite the cessation of sedation. After neurologic consultation, a brain MRI was performed which showed evidence of CPM in the pons. Despite supportive therapy, the patient did not show an improvement of mental status and after a 55-day hospitalization in the ICU she died from septic complications.The etiology of CPM is multifactorial, with liver transplant recipients being at an increased risk. Supportive treatment is the standard of care, and there are not enough evidence supporting other types of treatment.
Continue reading